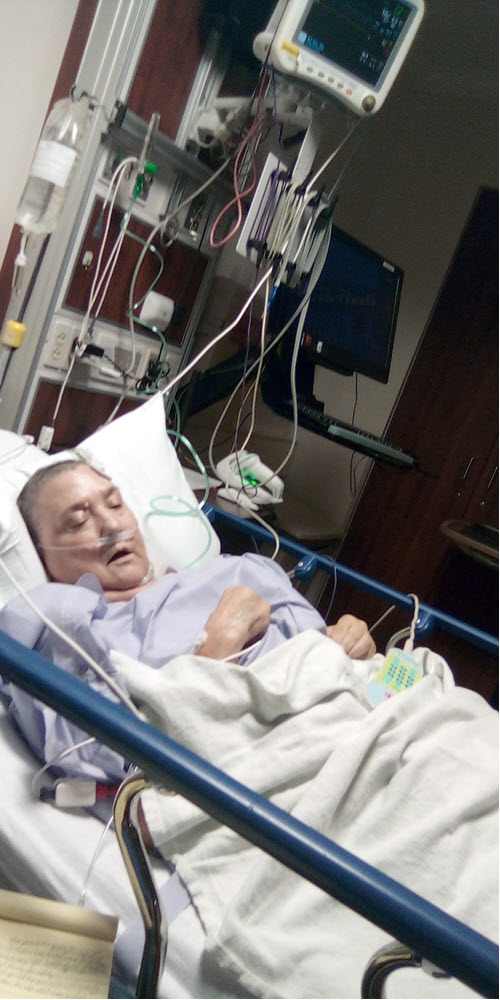
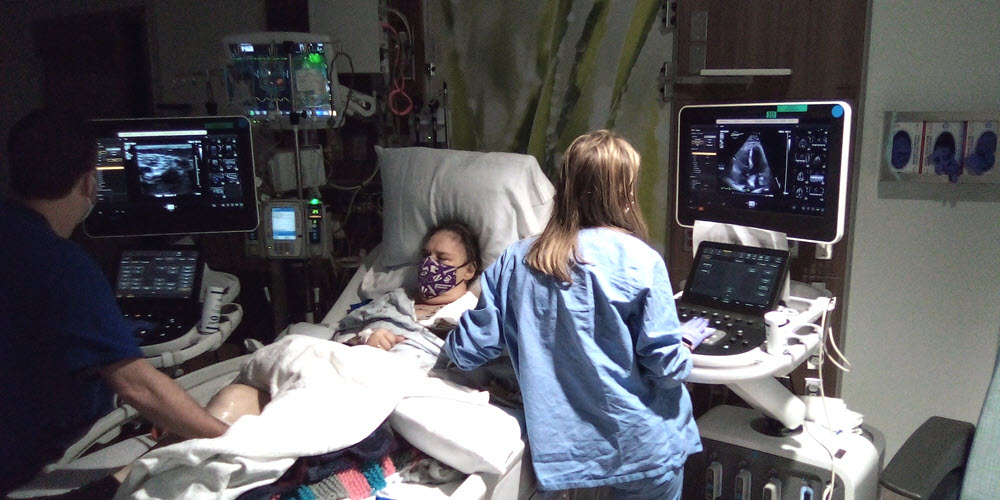
I really shouldn’t even be alive, but, by the grace of God, I’m now beating inflammatory breast cancer, having endured 14 surgeries, weeks of hospitalizations, 22 days of two-a-day radiation treatments and seemingly countless rounds of chemotherapy. Without MD Anderson’s Morgan Welch Inflammatory Breast Cancer Clinic, as well as Terry Arnold and The IBC Network Foundation, I no doubt would have succumbed by now to this very rare, uber-aggressive cancer.
In late summer 2022, about 2 1/2 years after I’d completed radiation for common HER2– invasive ductal carcinoma (IDC) of the right breast, I began noticing an itchy rash on my left breast. My oncologist in Gainesville, Georgia, first thought it was an allergic reaction to the adjuvant letrozole I was taking, but he took me off those chemo pills and the rash persisted. The local oncologist next tried topical treatment with increasingly large tubes of Lotrisone jock itch cream. Finally, at a dermatologist, we insisted on a punch biopsy, which returned indication of a de novo cancer – IBC – even though mammograms showed nothing.
Thankfully, we were led to Terry and the IBC Network and quickly realized our best hope lay with the unique multimodal IBC clinic at MD Anderson, nearly 900 miles away in Houston. First, we had to overcome the hurdle of a demand for more than $45,000 for us to walk in the door at MD Anderson, as it was not in our insurance coverage network; the ultimate charge was less, but you only get one life. In November 2022, on our first of what would be several trips to Houston, the IBC diagnosis was confirmed by an all-star team led by medical oncologist Dr. Azadeh Nasrazadani, surgical oncologist Dr. Anthony Lucci and radiation oncologist Dr. Wendy Woodward.
For treatment of stage IIIB HER2+ IBC, I swiftly began the presurgical chemo routine of Docetaxel and Herceptin/Perjeta at University Cancer & Blood Center (UCBC) in Athens, Georgia, under Dr. Petros Nikolinakos, who had completed his fellowship at MD Anderson. I soon began developing serious side effects with high fevers, and, early morning Dec. 20, 2022, wound up collapsing on the emergency room lobby floor at Piedmont Athens Regional. I had multiple life-threatening conditions, including acute bilateral pulmonary emboli plus blood clots in legs, as well as a raging kidney infection and urethra blockage causing sepsis, and I had become diabetic.
By February 2023, after more Athens hospitalizations, I had worsening interstitial pneumonitis. My husband, by my side throughout, connected the dots to determine the taxane (Docetaxel) to likely be behind the pneumonitis, and the doctors removed taxanes from my regimen. The day after my 65th birthday, in April 2023, when providentially my Medicare and supplement had kicked in, I underwent a left breast mastectomy plus removal of 17 lymph nodes at MD Anderson. At the same time, the team of Dr. Ashleigh Francis completed two microsurgical lymphovenous bypasses (LVBs), which, along with physical therapy and exercise, to date have fortunately staved off lymphedema.
After several Athens surgeries failed to resolve a life-threatening matrix stone that had infiltrated my left kidney, we were led to Houston Methodist Hospital, where, in late May 2023, Dr. Monica Morgan performed a percutaneous nephrolithotomy (PCNL) to remove what she described as a weird non-textbook fungal ball and protein matrix from the kidney. This cleared the way for the two-a-day radiation treatments to commence at MD Anderson while we lived for a second month out of the Best Western Galleria in Houston.
In April 2024, a year after my mastectomy, I got to ring another bell, after completing post-surgery chemo at UCBC, and, while a couple of subsequent Guardant Reveal liquid biopsies have shown small amounts of circulating tumor DNA, the latest test and scan show no concerns.
With a new healthier diet, I feel as well as ever and am blessed to be confident in the future. Whereas my experience, with such serious complications, may be unusual, initial misdiagnoses are commonplace with IBC, so it truly pays to do your own research and be persistent with providers. Moreover, it is imperative to get the best care possible, both at MD Anderson’s dedicated IBC clinic and locally.
A few other thoughts for the IBC journey:
- Keep meticulous detailed notes of all things medical and, preferably with the aid of a spouse or other individual, thoroughly research what may be going on and openly communicate with providers.
- For strength during radiation, as well as to promote hair coming back to one’s bald head, drink protein shakes (such as Muscle Milk, Pure Protein and Ensure Max Protein), two per day during radiation and one a day thereafter.
- While in Houston for radiation and otherwise, try to challenge yourself to do some fun things, from Astros baseball to evening bat-watching at the Waugh Drive Bridge and even the National Museum of Funeral History.
- Avail yourself of support through The IBC Network Foundation.
- Above all, prayerfully find the path the Lord has set forth and – even when it is a major struggle – follow that path faithfully, supported by the prayers of others.